
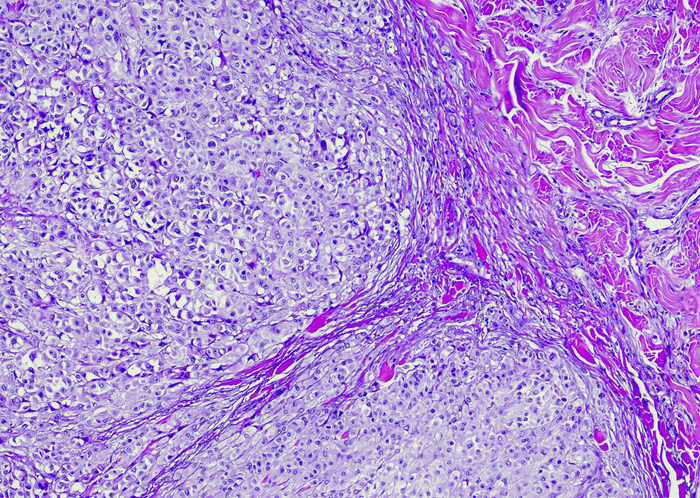
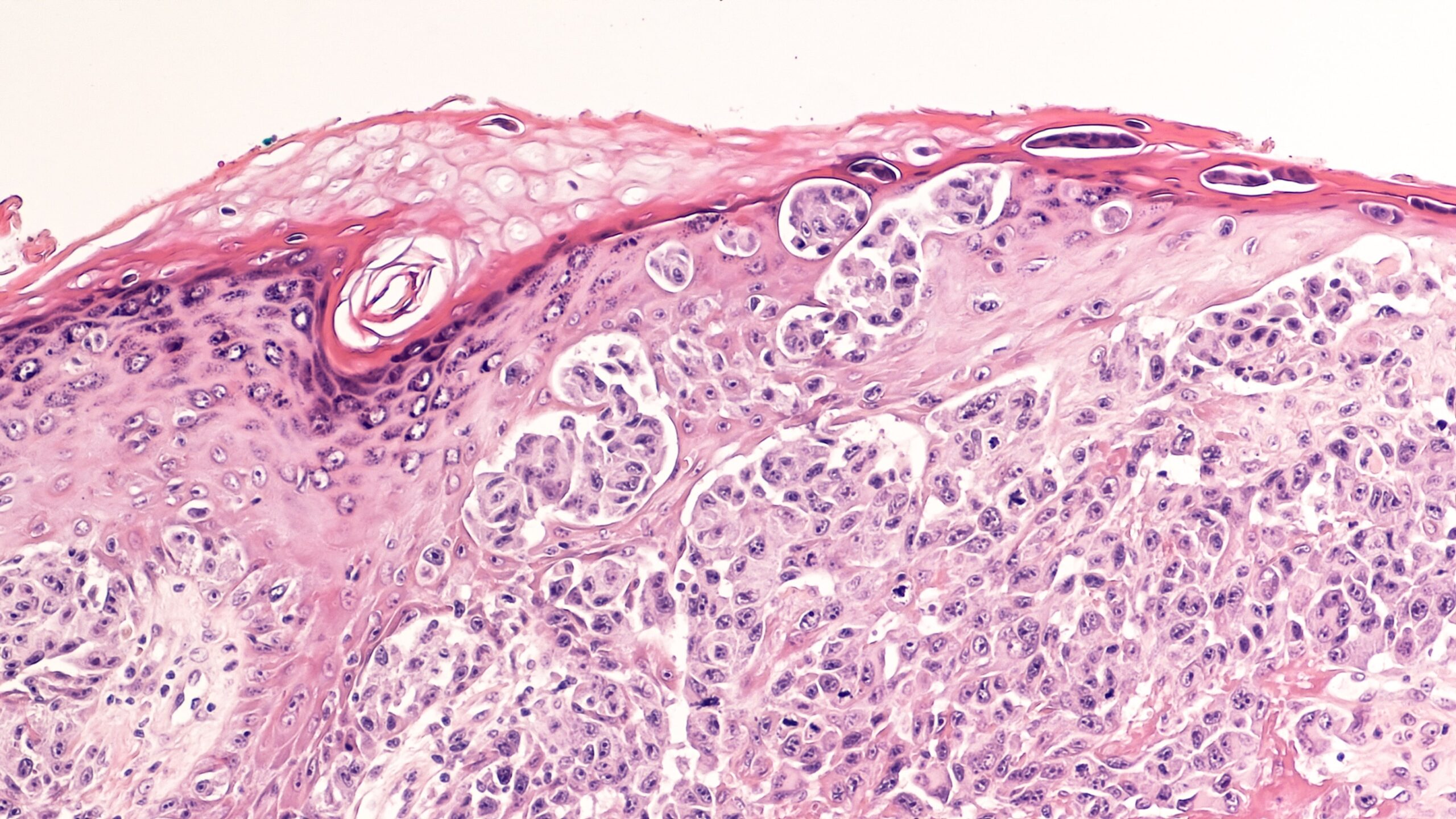
A study published in Clinical Cancer Research found that baseline levels of circulating tumor DNA (ctDNA) successfully predicted responses to first-line, but not second-line, immunotherapy for melanoma.
Levels of CtDNA, which can be detected in the bloodstream, have previously been found to correlate with response to targeted therapies for melanoma, though the relationship between responses to immunotherapy had not yet been established.
Researchers examined baseline ctDNA levels and immunotherapy outcomes in 125 adults with metastatic melanoma. 32 patients were treated with first-line immune checkpoint inhibition, while 27 patients received immune checkpoint inhibition in the second-line setting. The 66 remaining patients instead received first-line treatment with targeted therapy rather than immunotherapy.
Patients with low baseline ctDNA levels (fewer than or equal to 20 copies per milliliter) who received targeted therapy achieved longer progression-free survival (PFS) than those with high baseline ctDNA levels (greater than 20 copies per milliliter), in line with previous findings. For patients treated with first-line immunotherapy, those with low baseline ctDNA levels had an 80% longer PFS than those with high ctDNA levels. Association between low ctDNA levels and PFS remained after controlling for factors such as sex, age, tumor stage, BRAF mutation status, and brain metastases. Researchers found no significant association between baseline ctDNA levels and PFS in patients who received second-line immunotherapy, however.
Results were verified in a separate validation cohort of 128 patients with melanoma, who received either first- or second-line immune checkpoint inhibition (77 vs. 51 patients, respectively). In this group, patients with low baseline ctDNA who received first-line immunotherapy achieved a 58% longer PFS than those with high ctDNA levels, independent of sex, age, tumor stage, BRAF mutation status, and brain metastases.
“Our results indicate that it is necessary to carefully consider context when implementing biomarkers,” lead author Elin Gray, PhD, said in a press release. “ctDNA is often heralded as a good prognostic biomarker, but we found that this is not the case for patients receiving immune checkpoint inhibitors in the second-line setting…We need more of these kinds of studies evaluating the accuracy of ctDNA in various disease contexts, particularly now that liquid biopsy and ctDNA are being increasingly incorporated into the clinic.”


 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.