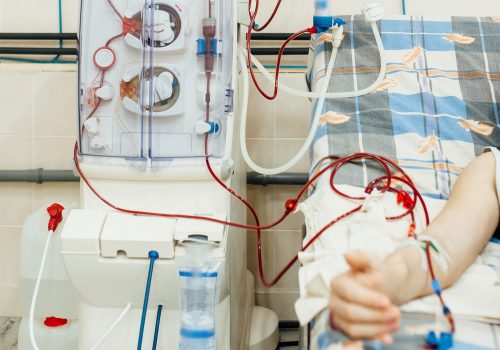
Acute kidney injury (AKI) is reported in up to 20% of all hospitalized patients and in 30% to 50% of hospitalized patients admitted to the intensive care unit (ICU). Even in mild disease, AKI is linked to increased rates of in-hospital mortality. Among hospitalized patients with severe AKI requiring renal replacement therapy (RRT), the mortality rate is an estimated 33% overall, and can be as high as >50% in patients in the ICU. The only FDA-approved therapy for AKI is RRT and continuous RRT (CRRT) is the preferred modality in the ICU due to an association with less hemodynamic instability compared with intermittent therapy.
The optimal dose in CRRT is based on urea clearance. In the 2012 Kidney Disease Improving Global Outcomes (KDIGO) clinical practice guidelines, the recommendations call for patients treated with CRRT to receive an effluent flow rate of 20 to 25 mL/kg/hour; the recommendation had a 1A rating. In 2013, the National Kidney Foundation Kidney Disease Outcomes Quality Initiative endorsed the recommendation for a CRRT dose of 20 to 25 mL/kg/hour.
However, according to Benjamin R. Griffin, MD, and colleagues, despite clear recommendations, dosing of CRRT remains highly variable. Results of national surveys reveal that <50% of practitioners target a specific dose, and only 15% of patients have regular dose assessments. In a preliminary data review at the University of Colorado Hospital (UCH), the average daily delivered dose of CRRT after accounting for machine downtime was not routinely documented; the prescription patterns also differed widely among nephrology faculty.
Dr. Griffin et al. designed a quality improvement initiative aimed at standardizing CRRT treatments at UCH. The researchers sought to increase the percentage of daily CRRT sessions within the target range of 20 to 25 mL/kg/hour to at least 65% within 1 year. The initiative and results were reported in the American Journal of Kidney Diseases [2019;74(6):727-735].
Participants in the initiative were adult patients treated with CRRT at the UCH between January 2016 and October 2017. The primary objective outcome measure was the percentage of treatments per week in which the average daily dose of CRRT was 20 to 25 mL/kg/hour. Secondary measures included mortality, number of CRRT treatments, length of stay in the ICU, and length of stay in the hospital. The average CRRT dose and compliance rates specifically on the first day of treatment were also recorded.
An assessment of the magnitude of the variability in CRRT dosing and four specific interventions were implemented during the course of 1 year: (1) modification of the electronic medical record (EMR) to include calculated average 24-hour dose in real time; (2) modification of the CRRT procedure note to include comments on dosing; (3) modification of the CRRT order set to display calculations; and (4) yearly educational sessions for renal fellows outlining CRRT specific dosing targets.
Prior to implementation of the interventions, dosing data from January to October 2016 were collected. During that time period, 915 treatment sessions were identified. Of those, 78 treatment sessions were excluded due to missing data, resulting in 837 sessions to analyze.
The average dose was 26.1 mL/kg/hour (standard deviation, 7.4). Of the 837 sessions, 33% (n=279) were between 20 and 25 mL/kg/hour; 21% (n=173) were <20 mL/kg/hour; and 46% (n=385) were >25 mL/kg/hour. In the group with an above-goal dose, 22% (n=187) were >30 mL/kg/hour and 2% (n=21) were >50 mL/kg/hour.
In terms of age, sex, and race, the populations of patients undergoing CRRT at UCH before and after implementation of the interventions were similar. The cause of AKI was also similar; sepsis was the leading cause of AKI in both populations. Also comparable were the ICU locations of treatment; the medical ICU accounted for the largest percentage of treatments in both populations.
In the post intervention group, the indications for CRRT were collected; patients nearly universally had stage 2 or 3 AKI by the KDIGO definition, and oliguria/anuria and volume overload were the most common reasons for CRRT.
Between February and October 2017, data on 952 treatments were collected. Following the interventions, 66% (n=631) of treatments achieved the goal dose. There was a substantial decline in the number of underdose treatments: 12% (n=113) received doses <20 mL/kg/hour. There was also a decline in the number of overdoses treatments: 22% (n=209) of patients received doses >25 mL/kg/hour. Only 4% (n=37) had doses >30 mL/kg/hour, and there were no treatments with an extremely above-goal dose (>50 mL/kg/hour). There was a notable decrease in week-to-week variance in dosing.
In terms of secondary outcomes, there was a statistically significant decrease in mortality: 60% preintervention versus 45% postintervention. There were no differences in days of CRRT treatment, length of stay in the ICU, or length of stay in the hospital.
Limitations to the study included the single-center design, potentially limiting the generalizability of the findings to institutions with different CRRT nursing models or different EMR systems.
In conclusion, the authors said, “An important component of CRRT delivery is ensuring that patients on CRRT receive an average effluent dose of 20 to 25 mL/kg/hour. Using a series of interventions including changes to the EMR, changes in documentation templates, and specific education of renal fellows, we were able to double our institution’s rate of dosing compliance.”
Takeaway Points
- There is wide variation in practice patterns of dosing of continuous renal replacement therapy (CRRT) in patients in the intensive care unit with acute kidney injury. A quality improvement initiation was implemented at the University of Colorado Hospital.
- The initiative sought to standardize CRRT practice patterns and reduce dosing variability; the primary outcome measure was the weekly percentage of CRRT treatments with an average delivered daily dose of 20 to 25 mL/kg/hour.
- Following implementation of the interventions, the rate of appropriate CRRT dosing was doubled and dosing variability was reduced.






 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.