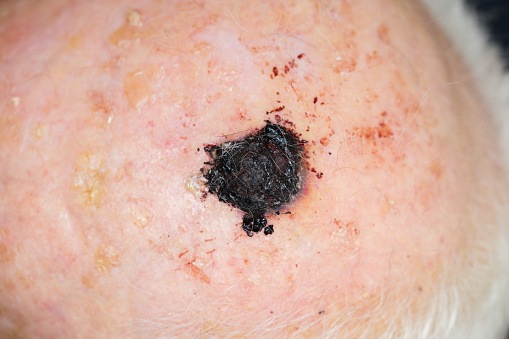
Recent research has found that vitamin D intake can reduce the aggressiveness of melanoma cells. This study, conducted by researchers from the University of Leeds, found that vitamin D influenced a signaling pathway within melanoma cells that slowed their growth and stopped their spreading to the lungs of mice. This work was published on November 5 in the journal Cancer Research.
Fortunately for the 16,000 new cases of melanoma diagnosed annually in the UK, the survival has doubled in the UK in the last four decades. Roughly 300 patients are diagnosed with melanoma in its most advanced stage each year in England, at which point the disease is particularly aggressive and difficult to treat. Around 55% of patients with this late-stage melanoma survive for one year or more, whereas nearly all of those diagnosed at the earliest stage survive to this point.
Previous research has suggested that lower vitamin D levels are correlated to poorer outcomes in melanoma patients, but the mechanism underlying this connection is not well understood. Professor Julia Newton-Bishop from the University of Leeds and her colleagues conducted this study to better understand what processes are regulated by vitamin D in melanoma cells and what happens when melanoma cells lack a vitamin D receptor (VDR).
Background of the University of Leeds Study
Netwon-Bishop and her team looked at the expression of the VDR-coding gene in 703 human melanoma tumors and in 353 human melanoma tumors that had metastasized or spread from their primary site. VDR expression was then cross-referenced with other patient data like the tumor thickness and speed of growth. They also wanted to see if the VDR concentrations in human melanoma cells were correlated to the genetic changes occurring as the tumor becomes more aggressive. Mouse models were then used to assess whether VDR concentrations altered the cancer’s ability to spread.
It was found that the human tumors with lower levels of the VDR gene spread faster and had decreased activity in genes that control immune pathways that combat cancer cells. The team also noted that the tumors with lower levels of VDR expressed higher activity in oncogenes or those linked to cancer growth and development. Specifically, upregulation was seen in the genes controlling the Wnt/β-catenin signaling pathway, which plays a role in cell growth.
In the animal models, the team noted that increasing the number of VDRs on the melanoma cells decreased the activity of this cancer-promoting Wnt/β-catenin pathway, slowing melanoma cell growth. These cells were less likely to form metastases in the lungs as well.
“After years of research, we finally know how vitamin D works with VDR to influence the behaviour of melanoma cells by reducing activity of the Wnt/β-catenin pathway,” Newton-Bishop said. “This new puzzle piece will help us better understand how melanoma grows and spreads, and hopefully find new targets to control it. But what’s really intriguing, is that we can now see how vitamin D might help the immune system fight cancer.
“We know when the Wnt/β-catenin pathway is active in melanoma, it can dampen down the immune response causing fewer immune cells to reach the inside of the tumour, where they could potentially fight the cancer better,” she continued. “Although vitamin D on its own won’t treat cancer, we could take insights from the way it works to boost the effects of immunotherapy, which uses the immune system to find and attack cancer cells.”
“Vitamin D is important for our muscle and bone health and the NHS already recommends getting 10 micrograms per day as part of our diet or as supplements, especially in the winter months,” explained Martin Ledwick, Head Information Nurse at Cancer Research UK. “People who have been newly diagnosed with melanoma should have their vitamin D levels checked and managed accordingly. If you are worried about your vitamin D levels, it’s best to speak to your doctor who can help ensure you are not deficient.”
Vitamin D dials down aggression in melanoma cells by influencing the behavior of a signaling pathway w/in melanoma cells, which slowed down their growth & stopped them from spreading @docmmiller https://t.co/cyKxoRqd2D via @medical_xpress
— delthia ricks ? (@DelthiaRicks) November 7, 2019



 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.