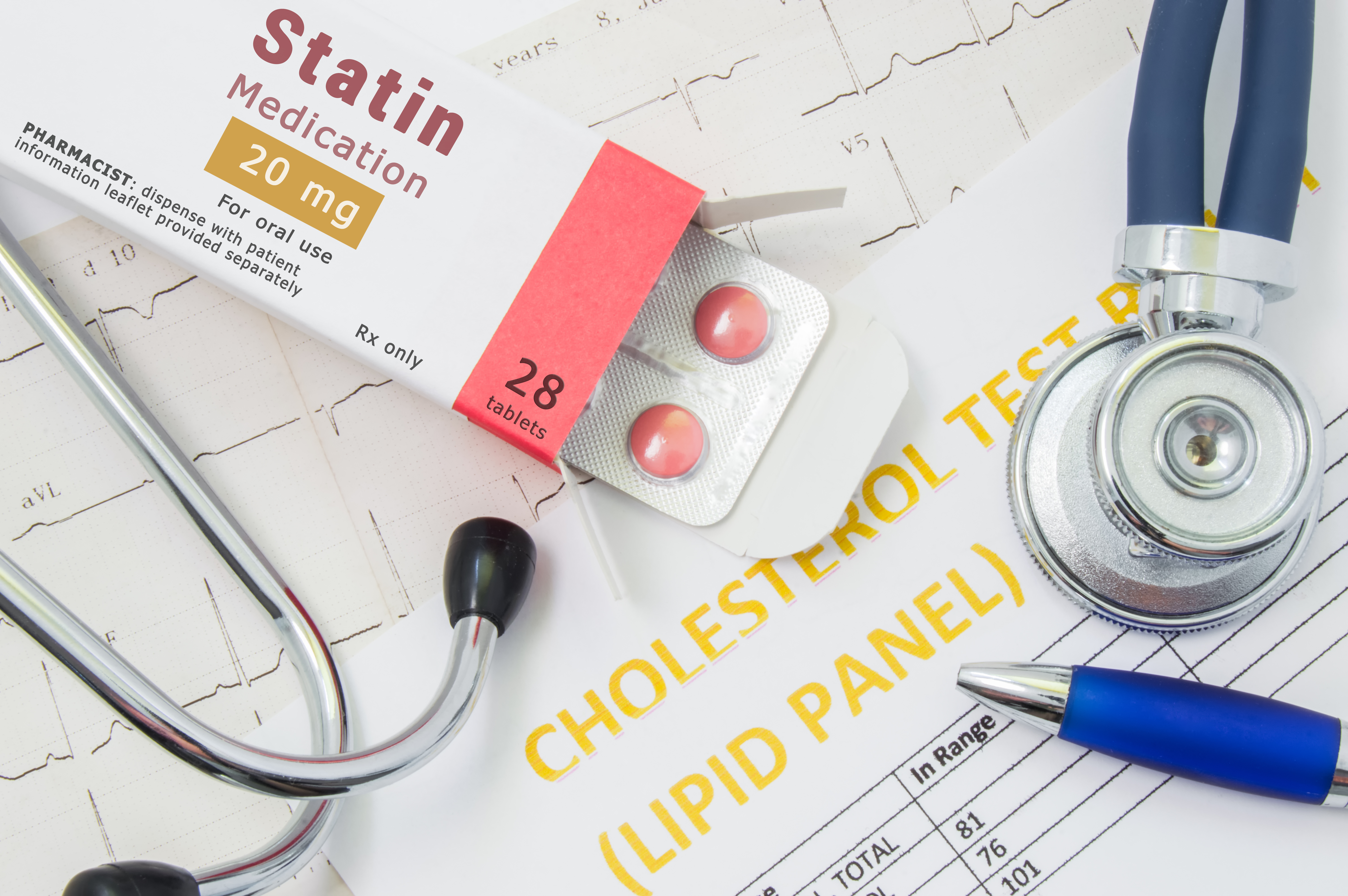
A new retrospective analysis suggests that older individuals taking statins had a 25% decreased risk for death than those not taking statins.
“Data are limited regarding statin therapy for primary prevention of atherosclerotic cardiovascular disease in adults 75 years and older,” the authors wrote.
The study included data on patients aged 75 years or older from the Veterans Health Administration who were free of atherosclerotic cardiovascular disease, and who had a clinical visit between 2002 and 2012. Data were linked with Medicare and Medicaid claims as well as pharmaceutical data, and excluded those with prior statin use. The authors used Cox proportional hazards models to evaluate the link between statin use and outcomes, and conducted propensity score overlap weighting for the balance of baseline characteristics. Outcomes of interest included all-cause and cardiovascular mortality, and secondary outcomes included composite atherosclerotic cardiovascular disease events such as myocardial infarction, ischemic stroke, revascularization with coronary artery bypass graft surgery or PCI. Mean follow-up was 6.8 years.
According to the study results, more than 57,000 patients were newly initiated statin users during the study period. There were 53,296 reported cardiovascular deaths, with 22.6 and 25.7 cardiovascular deaths per 1,000 person-years, respectively, among users vs. non-users. For the composite atherosclerotic cardiovascular disease outcome, there were 66.3 and 70.4 events per 1,000 person-years, respectively, for users versus non-users. Following propensity score overlap weighting, the hazard ratio was 0.75 (95% CI, 0.74 to 0.76) for all-cause mortality, 0.80 (95% Ci, 0.78 to 0.81) for cardiovascular mortality, and 0.92 (95% CI, 0.91 to 0.94) for the composite atherosclerotic cardiovascular disease events in statin users versus non-users.
“Based on these data, age is not a reason to not prescribe statins,” lead author Ariela Orkaby, MD, MPH, a physician scientist at VA Boston Health Care System and in the Division of Aging at the Brigham, said in a press release about the study. “Statins are commonly studied and prescribed for middle-aged adults but understudied in people over age 75. One of the most remarkable things about our results is that we found the benefit of statins held true regardless of whether a person was older or younger or had a condition such as dementia.”
Dr. Orkaby also noted some study limitations.
“There are many interesting leads to follow up on, but it’s important to keep in mind that this is not a randomized, clinical trial,” she added. “Instead, it’s a retrospective analysis using real world data that helps us explore where the truth lies.”
The study was published in JAMA.
Important work by @DrAROrkaby and team using @DeptVetAffairs data. Great support for #PREVENTABLE RCT! https://t.co/d8z7IYr63y https://t.co/xJV9LE7AOb
— Scott Hummel (@SHummelMD) July 7, 2020
Significant findings that call for randomized controlled trials examining the safety and efficacy of statins in adults 75+ y.o. As usual, must always weigh harms with benefits, but strong evidence to not discontinue statins based on age alone. @geronsociety @AmerGeriatrics https://t.co/Zc4L52K20h
— Clark DuMontier, MD, MPH (@cdumonti) July 7, 2020
Using VA data we found a 25% reduction in all-cause mortality and 20% reduction in CV-mortality in new statin users >75 years. Same in those >90 and with dementia. Age should not be a reason to withhold statins! https://t.co/FGuZI7aXuP@JAMA_current @VAResearch @BrighamAging
— Ariela Orkaby MD MPH (@DrAROrkaby) July 7, 2020






 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.