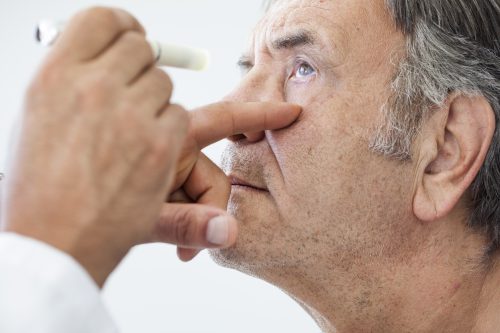
Diabetic retinopathy was a hot topic at AAO 2019, and two new research papers presented at the meeting explore the aspects of the
The first, “What Happens to Diabetic Retinopathy Severity Scores with Less Aggressive Treatment? A Post Hoc Analysis of the RISE/RIDE Open-Label Extension Study,” sought to find how less-than-monthly therapy following monthly ranibizumab would affect Diabetic Retinopathy Severity Scores (DRSS). Here, researchers conducted a post-hoc analysis from the RISE/RIDE open label extension (OLE). Clinical treatment and patient characteristics were analyzed by patients whose DRSS stabilized or improved compared to those whose DRSS worsened. Final analysis included 367 patients, of whom 263 (72%) had stabilized or improved DRSS. Maintenance and improved eyes received an average of 4.4 injections during the p.r.n. period, compared to 2.3 injections in the group whose DRSS worsened. Of those whose DRSS improved during RISE/RIDE, 108 (55%) maintained or improved DRSS with less-than-monthly therapy. The authors concluded that while the majority of patients were okay with less-than-monthly treatments to maintain their DRSS, “some minimum treatment may be necessary for DRSS stability.”
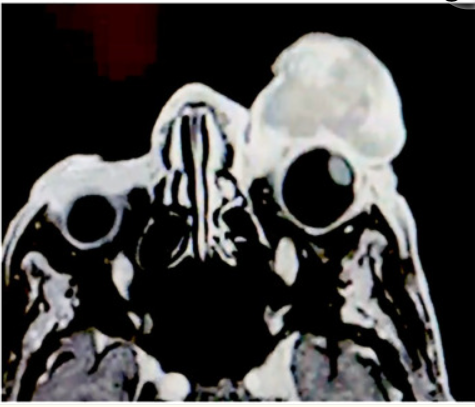
The second study assessed the correlation between obstructive sleep apnea (OSA) and diabetic macular edema (DME) and how OSA affects DME in patients with type 2 diabetes mellitus (T2DM). T2DM patients who received both OCT and polysomnography (PSG) between June 1, 2009, and June 1, 2017, were included in the trial. Refractory DME was defined as more than three times of therapeutic solutions. Final analysis included 97 eyes (51 patients), which were stratified by with (n = 31) or without (n = 66) DME. A significant relationship was observed between severe OSA and DME. Severe OSA patients were significantly more likely to present refractory DME than nonsevere OSA patients. The authors concluded by citing severe OSA as a risk factor for DME and a precursor to refractory DME.




 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.