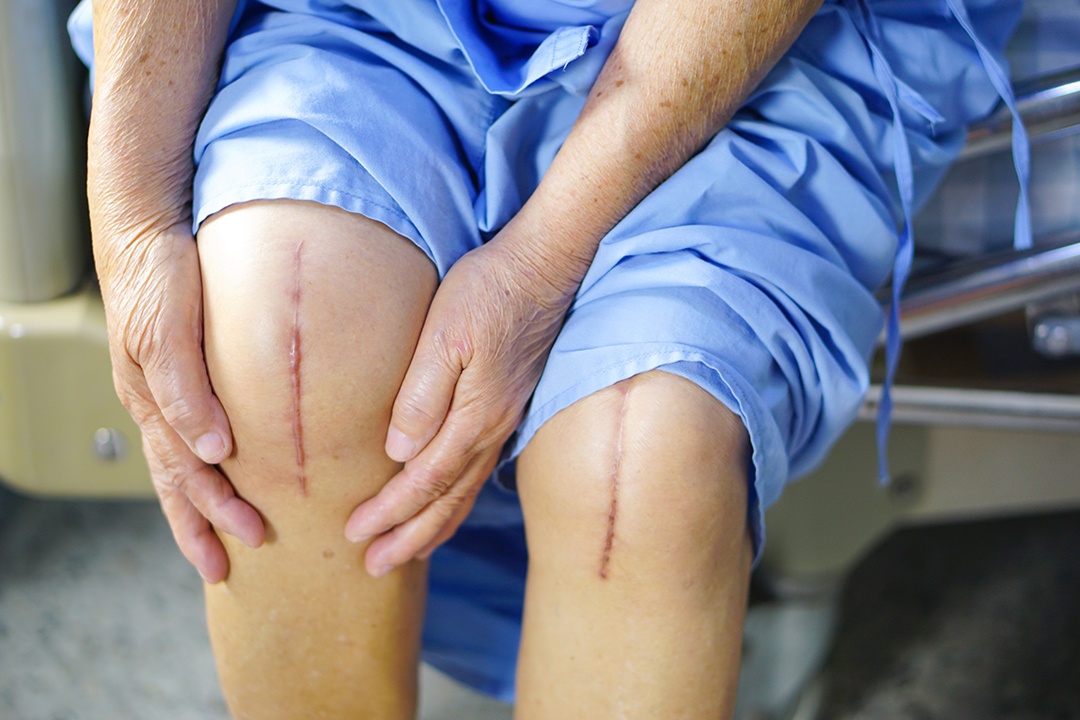
Knee arthroscopy may be performed prior to total knee arthroplasty (TKA) in patients with symptomatic degenerative knee changes that do not yet warrant TKA. A study published in The Journal of Bone & Joint Surgery observed that time between knee arthroscopy and TKA impacts the prevalence of revision surgery and postoperative periprosthetic joint infection (PJI).
Researchers assessed whether the time interval between knee arthroscopy and subsequent primary TKA is associated with increased rates of revision and certain complications following TKA. A national insurance database was used to identify patients who underwent knee arthroscopy within one year prior to primary TKA between 2006 and 2017. Patients were stratified into cohorts based on time from knee arthroscopy to TKA: 0 to 15 weeks, 16 to 35 weeks, 36 to 43 weeks, and 44 to 52 weeks. Univariate and multivariable analyses were conducted to determine the association between these specific time intervals and rates of revision surgery, PJI, aseptic loosening, and manipulation under anesthesia.
The study included 130,128 patients: 6,105 (4.7%) underwent knee arthroscopy within one year prior to TKA and 124,023 (95.3%) underwent TKA without any prior knee surgery, including arthroscopy (control group). Compared with the control group, the likelihood of undergoing revision surgery was significantly greater in patients who underwent knee arthroscopy ≤15 weeks (odds ratio [OR], 1.79; 95% confidence interval [CI], 1.43-2.22; P<0.001) or 16 to 35 weeks (OR, 1.20; 95% CI, 1.01-1.42; P=0.035) prior to TKA.
Risk of PJI significantly increased if knee arthroscopy was performed ≤35 weeks prior to TKA. Among patients who underwent knee arthroscopy within one year before TKA, all four time cohorts had an increased risk for manipulation under anesthesia.
“This study suggests that an interval of at least 36 weeks should be maintained between the two procedures to minimize risks of PJI and revision surgery,” the researchers concluded.




 © 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.
© 2025 Mashup Media, LLC, a Formedics Property. All Rights Reserved.